Diastasis Recti and Constipation | Two Common Postpartum Body Challenges
Written by: Kim Vopni, The Vagina Coach.
Est. reading time: 9 minutes.
There are two things that I will never forget about the early hours after giving birth to my first son Diastasis Recti and Constipation.
I remember how disconnected my upper body felt from my lower body when I got up to go to the bathroom for the first time after my baby entered the world. I felt like I had to hold myself together.
There are two things that I will never forget about the early hours after giving birth to my first son Diastasis Recti and Constipation.
I remember how disconnected my upper body felt from my lower body when I got up to go to the bathroom for the first time after my baby entered the world. I felt like I had to hold myself together.
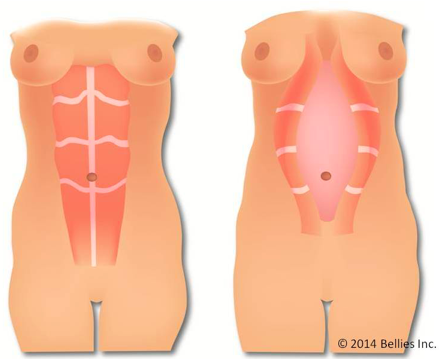
What was a fairly tight compact part of my body, was now a vacant space with very little tone. The muscles in my abdominal wall had stretched well beyond their normal, optimal length and the rectus muscles (think 6 pack) had also moved away from their midline position – a condition known as diastasis recti.
As I sat down to pee, I had a sudden panic attack knowing that at some point I was also going to have to poop!
The thought of that first bowel movement after giving birth is almost scarier than the birth itself! This fear coupled with other influences I will elaborate on below, can contribute to postpartum constipation.
Diastasis Recti and constipation are very common and with the right information, can be very well managed and don’t have to be a big deal in the early postpartum period or beyond. Let’s look first at constipation.
Postpartum Constipation
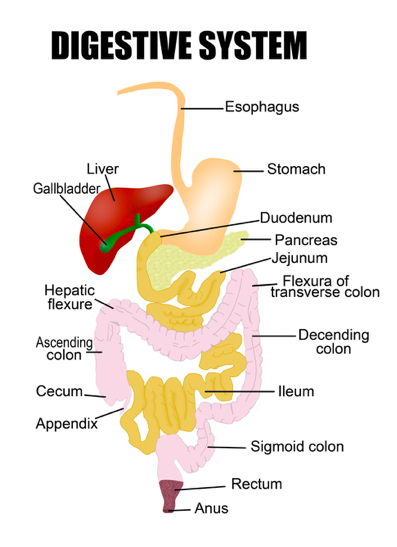
Labour typically slows down the digestive system, especially if you had an epidural and it can take a few days to get back on track. Other things that can influence the digestive system in the early weeks postpartum are pain medications, iron supplementation and fear of pooping.
A lot happens in the pelvis and to the vagina, perineum and anus – things like tearing, stitches, tenderness and hemorrhoids. The thought of anything else passing through can be a bit stressful to say the least. Stress activates the ‘fight or flight’ response which reduces blood flow to the digestive system and can contribute to constipation.
From a Chinese medicine perspective the first system that needs to be addressed in postpartum healing is the digestive system. The digestive system is responsible for transforming food into blood and energy and if digestion is off, then the body will not benefit from the food consumed and therefore not build the blood and energy needed for healing.
Mother Roasting
It is also believed in Chinese Medicine that the body has ‘opened’ during pregnancy and birth and is therefore susceptible to ‘wind’ or ‘cold’. New mothers have a 30 day period of “sitting in” where the mother does not go out and is instead served warm soups, stews, and broths that are easy to digest.
Korea has a 100 day period where the mother and child do not leave the home. In Japan, the mother and baby stay at the mother’s parent’s home for some pampering and one-on-one time with the baby. India and African nations include traditions of 10-40 day isolations where additional support is provided including massage, childcare and food preparation.
Other practices from places like Malaysia include belly binding and hot stones on the abdomen to help cleanse it, close it and heal it.
These practices not only allow the body time to recover from the trauma of giving birth but provide a period of mental rest that I firmly believe creates a solid foundation for mom and baby from day one.

The belief of the need to ‘close’ the body is justified. Diastasis Recti has been shown to happen to 100% of women in the third trimester and the gap between the muscles doesn’t always return to its pre-pregnancy state, nor does the connective tissue naturally regain its supportive tensioning role in the core. The muscles in the pelvic floor have also stretched and in some cases have been cut or torn which can contribute to challenges with core control and continence.
Belly wrapping or belly binding aims to provide temporary compression and support to the pelvis and abdominal wall in the early weeks postpartum when the muscles are temporarily hindered in their ability to contribute to core control.
The muscles and connective tissue in the abdominal wall and pelvis are key with regards to stability and control in our inner core but so are the bones and joints. In the pelvis, the shape of the bones provides what is called ‘form closure’ while the muscles, ligaments and connective tissue contribute to what is called ‘force closure’. During pregnancy biomechanical changes occur in the body which can reduce the effectiveness of both form and force closure such as;
- Altered posture and load bearing;
- Altered muscle length in the pelvic floor and abdomen (both longer and shorter) which results in reduced ability for muscle force production;
- The role of relaxing and progesterone contribute to joint laxity and when the ligaments are lax it affects the force closure.
- The abdominal muscles are stretched to allow space for the enlarging uterus, which can lead to loss of muscle tone and strength in the abdominal region and a compromised ability to produce tension in the thoracolumbar fascia, resulting in reduced force closure in the pelvis;
- Diastasis recti is a distortion in the abdominal wall and can impair the function of the muscles including their role in posture and pelvic stability;
- The transversus abdominis, multifidus, diaphragm and the pelvic floor are all anticipatory muscles of the core and are required for force closure in the pelvis – all are affected by posture and alignment changes in pregnancy
- Intra-abdominal pressure – altered mechanics and alignment mean management of intra-abdominal pressure will change
The benfits of Castor Oil include these three main functions:nutrient-rich, pain-relieving and anti-inflammatory.
Add a Fascia Massage Roller to these benefitsand you’ve now super boosted these functions.
You see, combining Castor Oil to your Fascia Massage Roller practice helps to massage the tight tissues and adhesions found along energetic pathways that can become blocked by physical or emotional trauma.
And the benefits of this practice are:
- Breaking down of scar tissue from injury, cesarean section, surgery, and/or endometriosis
- Fade stretch marks from weight gain or postpartum
- Fascia release for sore muscles and tight IT bands
- Lymphatic drainage and circulation
- Support smoothing out cellulite
Sounds amazing, right?
Intra-Abdominal Pressure
We can’t talk about postpartum recovery and wrapping without talking about intra-abdominal pressure.
Intra-abdominal pressure is defined as the pressure within the abdominal cavity. It is part of our core stability system. We need some, but not too much and we need an ability to manage the varying pressures throughout the day. When we take a breath in, the diaphragm descends and there is a compression action on the abdominal contents which acts to stabilize the pelvis and spine. We can have too much pressure such as a Valsalva maneuverer which is an inhale, then breath hold while bearing down. This often results in a distended abdomen and can place pressure on the pelvic organs as well.

We can’t talk about postpartum recovery and wrapping without talking about intra-abdominal pressure.
Intra-abdominal pressure is defined as the pressure within the abdominal cavity. It is part of our core stability system. We need some, but not too much and we need an ability to manage the varying pressures throughout the day. When we take a breath in, the diaphragm descends and there is a compression action on the abdominal contents which acts to stabilize the pelvis and spine.
We can have too much pressure such as a Valsalva maneuverer which is an inhale, then breath hold while bearing down. This often results in a distended abdomen and can place pressure on the pelvic organs as well.
The reverse can also be seen in a technique called “hypopressives” which decreases intra-abdominal pressure and results in a hollowing or concavity of the abdomen. A reliance on one may result in a compromised ability to manage changes in intra-abdominal pressure such as during lifting or exercise.
Crunches were given a bad rap because they cause an increase in intra-abdominal pressure but a study found that activities like standing up from a chair or downward dog pose in yoga actually created equal or greater increases in intra-abdominal pressure which suggests that managing intra-abdominal pressure is more about HOW a person performs a movement or exercise rather than the exercise itself.
Wrapping is often considered to be a practice that increases intra-abdominal pressure and it can when done incorrectly. Wrapping is ideally done to temporarily contribute to force closure in the pelvis with some gentle hugging of the abdominal wall.
Many mistakenly wrap only the waist and wrap very tightly in hopes that it will help heal the gap between the abdominals (diastasis recti). Instead it increases intra-abdominal pressure, it interferes with digestion and it restricts optimal breathing patterns which can prevent healing of the abdominal wall and pelvic floor and can also contribute to constipation.
My recommendations for postpartum recovery include principles that support rest and belly wrapping in the early weeks postpartum, core retraining with pelvic floor initiated movements, a balance between hyper and hypopressive exercise and nutrition that is based on the traditional practices of mother roasting to support optimal digestion.
Are you a practitioner, health coach or wellness influencer? If you’re interested in recommending our easy-to-use tools and practically applying them in your health and wellness professional practice in clinic or online with the people you serve or become a wholesale partner:
Disclaimer
Disclaimer: Any opinions, advice, statements, services, offers, information or content expressed or made available by third parties, including information providers, are those of the respective authors or distributors. Neither Queen of the Thrones® nor any third-party provider of information guarantees the accuracy, completeness, or usefulness of any content. This communication does not create a doctor-patient relationship. Information provided does not replace the advice of your health care practitioner. If you happen to purchase anything we promote, in this or any of our communications, it’s likely Queen of the Thrones® will receive some kind of affiliate compensation. Still, we only promote content and products that we truly believe in and share with our friends, family and patients. If you ever have a concern with anything we share, please let us know at care@queenofthethrones.com. We want to make sure we are always serving Our Queendom at the highest level.



0 Comments